Background
Cluster of wound botulism in injecting drug users
- Information from National Disease Surveillance Centre
- Sporadic cases have been peported in IV drug users
- All cases had a flaccid paralysis
- Drugs contaminated with the anaerobic Clostridium botulinum
Abroad
- Several people had (2023, France) botulism poisoning from eating contaminated food
- In the USA, botulism is associated with skin popping "black tar" heroin
Causative organism
- Symptoms of botulism are caused by a toxin produced by the gram +ve, anaerobic, spore forming Clostridium botulinum
- The toxin blocks the release of acetylcholine at the neuromuscular junction → descending flaccid paralysis
- Botulism is not spread from one person to another
- There are three naturally occurring forms of botulism:
- Food-borne botulism, caused by ingestion of pre-formed toxin
- Wound botulism, which occurs when C. botulinium spores contaminate a wound, germinate and produce toxin in vivo
- Intestinal colonisation botulism, usually seen in infants
Clinical features
Afebrile
Descending
Flaccid Paralysis
Patients with botulism typically present with:
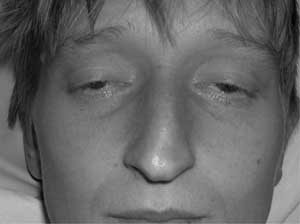
- Difficulty speaking, seeing and/or swallowing
- May have double vision, blurred vision, drooping eyelids
- Slurred speech, difficulty swallowing, and muscle weakness (later, loss of tendon reflexes)
- Paralysis may progress to the arms, legs, trunk and respiratory muscles
- Usually no fever
- No loss of sensation
- No loss of awareness
There may also be autonomic signs with:
- Dry mouth, fixed or dilated pupils
- Cardiovascular, GI and urinary dysfunction
If onset is very rapid, there may be no symptoms before sudden respiratory paralysis occurs, which may be fatal. Recovery can take months.
Differential Dx of BOTULISM
- Guillain Barré
- Usually ascending motor paralysis
- Miller Fisher (Guillain Barré variant):
- May be descending, paralysis ± bulbar
- Organophosphate poisoning
- Myaesthenia gravis:
- Fatiguability, better at rest
- Lambert Eaton syndrome:
- Proximal muscle weakness (not face)
- Paralytic shellfish poisoning
- Tick paralysis
- Encephalitides
- Enterovirus infection
Laboratory
Confirmation of the clinical diagnosis is by the demonstration of botulinum toxin in blood samples or, in the case of wound botulism, by the identification of C. botulinum in wound specimens. Specimens should be sent immediately to the reference laboratory.
Samples to be taken from acutely ill patients include:
- Serum. At least 10ml. Serum samples must be collected before antitoxin is administered
- Wound. Pus. As much as possible in a sterile container. If no pus - swab in anaerobic culture medium.)
- Biopsy tissues. If surgical debridement is performed, biopsy tissues should be placed immediately into a sterile container
- Post mortem specimens. Heart blood (10ml), if not haemolysed, should be sent for serum for serum collection. Specimens from infected wounds may also be useful
- All samples must be kept refrigerated after collection
- Specimens should be sent directly to the reference laboratory with the sender’s name and address clearly marked. Call the reference laboratory prior to sending the sample
Clinical management
Botulism Antitoxin
Botulism anti-toxin (if required) can be procured by contacting: Dr Seamus O’Dea, Cherry Orchard
Tel 01 620 6000 (or medical officer on call)
- Specialist advice should be urgently sought from ID or Micro
- Botulinum antitoxin is effective in reducing the severity of symptoms if administered early in the course of the disease
- C. botulinum is sensitive to benzyl penicillin and metronidazole
- In cases of wound infection, antimicrobial therapy and surgical debridement should reduce the organism load and therefore toxin production, but circulating toxin can only be neutralised by the early administration of antitoxin
- Beware respiratory fatigue - regular blood gases and spirometry (intubate if ↓O2 or ↑CO2 or FVC < 30%)
- Where there is definite clinical suspicion of botulism, treatment with antitoxin should not be delayed for microbiological testing
- Discuss with neurophysiology re nerve conduction studies in (well!) cases of suspected Miller Fisher
Reporting & public health investigation
- Food samples associated with suspected cases of food borne botulism must be obtained as a matter of extreme urgency in order to prevent further cases
- Reference for this page is : CEM/CMO/2002/14
Links
- National Disease Surveillance Centre Virus Reference Laboratory Belfield
- Please inform pharmacy that you are requesting the anti-toxin - it is an unlicensed product details at NIO site
- Botulism Antitoxin SPC
- Botulism Antitoxin product
- Botulism Antitoxin Local (HSE) version