Background
- Burns may be from flame, electricity, hot fluid, etc.,
- Classified as superficial, deep dermal or full thickness
- Classified as complex or simple
- Area estimated = rule of 9s in adult, burns charts in children
- 1% = area of the palm (excluding wrist but including fingers) in any agegroup
- Areas of erythema alone or soot covered unharmed skin are not included
- Major burns = > 15% in an adult or > 10% in a child/elderly
Complex burns
Age
- under 5yrs or over 60yrs
Site
- Face or hands or perineum or feet (with dermal or full thickness loss)
- any flexure (esp neck or axilla)
- circumferential dermal
- full thickness burn of the limbs/torso/neck
Inhalation injury
- Any significant such injury (excluding pure CO poisoning)
Mechanism of Injury
- Chemical injury, > 5% TBSA, exposure to ionizing radiation injury, high pressure steam injury
- High tension electrical injury, hydroflouric acid injury (> 1% TBSA)
- Suspicion of NAI
Age
- < 16 >5% TBSA (dermal or full thickness loss)
- Adult >10% TBSA
Basic principles of resuscitation and airway management. If you are worried about a burn, discuss it with the one of the EM consultants. They will see any burn you are concerned about. If it is a major burn, discuss with EM consultant before discussing with local burns unit. The majority of burns we see can be treated here in the ED.
Discuss all complex burns wiith the duty EM SpR or Consultant.
A burn may also be complex if it occurs with:
- Cardiac limitation and/or MI within 5yrs
- Respiratory limitation of exercise
- Diabetes, either IDDM or NIDDM
- Pregnancy
- Immuno-suppression for any reason
- Hepatic impairment; cirrhosis
- Associated injuries:
- Crush injuries
- Fractures
- Head injurie
- Penetrating injuries
Management Major burns
If possible smoke/thermal injury to respiratory tract or burns to head / neck - manage airway.
Treatment
- Seek help
- Clear and maintain airway - with C-spine cautions
- Give oxygen (high concentration)
- Check PEFR and give nebulizer if bronchospasm
- Consider RSI and intubation(sore throat, hoarse, carbaceous sputum)
- Check pulse, blood pressure and respirations
- Cannulate away from burn if possible
- Give IV crystalloid
- Do not insert a central line
- Administer analgesia
- Chart area involved Lund & Browder)
- Catheterise (accurate urine output)
Investigations
- ABG including COHb
- CXR
- FBC (PCV, Hb)
- X-match
- U&E, COHb
- Forensic serum sample
Obtain brief history
- Mechanism of injury (exclude co-existing trauma)
- Type of thermal injury
- AMPLE history
- Note time of burn
Examination notes
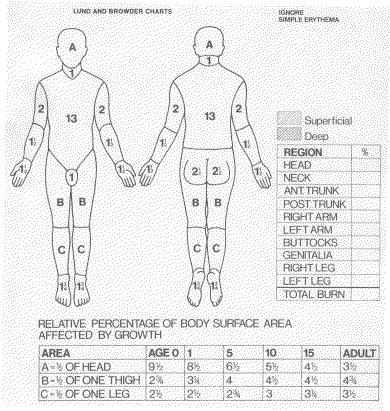
- Area: rule of 9's for adults, Lund & Browder chart for children
- Area of hand = 1%
- Depth of burn:
- History - electricity, epilepsy, ethanol and burnt clothing imply full thickness
- Record exact timings if possible
- Appearance - white discolouration / eschar suggest full thickness by pin-prick test
- General examination particularly for other signs of trauma
- Circumferential burns of a limb may cause severe compression with the risk of ischaemia; therefore always consider whether any escharotomy needs to be performed. If in doubt - ask!
- Apply sterile dry dressings, e.g. paraffin gauze or cling film
- Check tetanus cover
- Do not apply ointment
- Discuss with your ED senior before you contact a burns unit
Fluid management in major burns (Parkland formula)
- Hartmans 2ml/kg x weight x %burn in adults
- Hartmans 3 ml/kg x weight x %burn in children
- Fluid management should be guided by urinary output - Aim for a urine output of 1 ml / kg / hour
- Remember - these are in addition to normal fluid requirements
Burns in children
- Use the same ABC approach as above
- Remember children can decompensate very quickly
- Airway compromise is more common in children
- Use the paediatric burns body charts to estimate surface area of the burn
- Check for complex burn criteria
- Give analgesia early - intravenous morphine 0.1 mg / kg
- Lund & Browder chart
Transfer arrangements
Before transfer
- Ensure airway is safe
- Ensure IV lines are reliable, esp if long journey
- Keep warm, especially children
- Transfer with dry dressing or cling film, not wet towels
- Arrange appropriate escort
- Documentation
- Analgesia
Phone accepting hospital as you are leaving.
Minor burns
Discuss the management of full thickness burns (even if localised) with EM consultant.
- Transfer may be indicated according to anatomical site, e.g. face, hand, perineum
- Blisters should be left intact whenever possible for pain relief and to reduce infection. If bulk is a problem, aseptic aspiration is second choice. However, if a blister has burst and there is a layer of sloughed epidermis this should be removed and the exposed burn cleaned and dressed
- Apply vaseline ointment only to areas treated by exposure (face, perineum) and Bactroban or flamazine for occluded areas (hands)
- Alternatively the hands can be placed in a polythene bag containing Bactroban or flamazine
- Discuss with senior nursing staff
- To other areas apply sterile non-adherent dressing, e.g. Betadine on release with gauze to soak up exudate (and crepe to cover)
- Elevate all limb burns
- Check tetanus cover
- Review patients not requiring admission in the ED clinic (± lavage with 50:50 mix of Betadine and normal saline before similar dressings)
- New blisters may need to be managed as above.
- Wound depth is often best assessed 2 or 3 days after a burn
- Be wary of non-accidental injury
- Please discuss any cases needing plastics opinion with the on-call plastics team at CUH prior to completing the soft tissue clinic referral form
Watergel
- Watergel should be used if there is concern about ongoing burning
- Waterjel dressings are available in the resuscitation room ± store room in the ED
- Are water-based, sterile, bacteriostatic, non-toxic, non-adhesive burn dressings
- Can be applied over burnt clothing etc
- Aim of treatment is to cool the burn and not the patient!
- Indications for use include any area where there is a need for heat to be dissipated from body surface area
- Contra-indications include any dry ‘powder’ chemical contamination (needs to be brushed from area carefully) or any liquid chemical contaminants (almost all require irrigation for a minimum of 30 minutes)
- Waterjel dressings have the cooling capacity of up to 250L of water
- Can dissipate temperature up to 1100° C
- Vital to obtain a ‘pre-cooling’ history from the E.M.T. or witness
- Ensure to get as full a history as possible (both scene and patient history). For example, ascertain whether female patients are menstruating (in case of toxic shock syndrome from tampon use);
- Extremely useful in Tar/Bitumen, molten metal/glass/plastic burns,
- Apply dressing as usual, but may require more dressings
- Tar/bitumen etc, should harden and heat is removed from tar etc
- Useful in treatment of ‘jellyfish’ stings as dissipate heat
- Extra gel in the packs can also be used on area not covered by dressing, i.e. zone of hyperaemia
- Dressings may be removed as soon as burn is cooled (discuss with patient)
- Normal wash down procedures apply to Waterjel
Non acute referrals to local burns unit
- Wound healing any wound unhealed at 14 days post injury
- Complications any significant infection, septic episode or suggestion of a Toxic Shock-like illness
- Plastic surgery trauma clinic at CUH Referral Form
Rehabilitation
Conmsider early in wound where scarring suggests:
- A significant aesthetic impact and/or psychological disturbance
- The need to consider skin camouflage
- A significant functional limitation
- The need to consider pressure therapy or other forms of scar modification
- The need to consider surgical reconstruction
Specific types of burns
Burns to the face
- May pose upper airway oedema and obstruction
- In general, leave burns to the face exposed
- Clean twice a day
Supficial burns to the hand
- Should be treated with Bactroban in a polythene bag with daily dressings and the hands washed under the tap between dressings
- The use of Bactroban should not be too liberal
- The patient may need to have the dressing changed twice a day (a soggy, macerated mess, you are probably using too much Bactroban)
- Once the Bactroban and bag dressing is stopped the hand will dry and heal very quickly
Chemical
- With the rare exception of alkali metals which can explode in the presence of water (sodium, potassium, rubidium and caesium) irrigate copiously with water
- Beware of causing hypothermia in children
- Avoid neutralisation reactions (exothermic)
- Ca++ gluconate is indicated for hydrofluoric acid burns (topical gel and/or local injection). Alkali binds to the tissues and exerts its effect deceptively for some hours, so continue irrigation and refer to Burns Unit via your ED senior. Systemic toxicity is produced by hydrofluoric acid, phenols and yellow (white) phosphorus which ignites in air and must be covered by water or wet dressings. Hydrofluoric acid and phosphorus can both depress calcium levels which should be checked in larger burns
- Phenol can be removed from burns by swabbing with polyethylene glycol 300
Electrical
- More details in Environment - Electrocution page
- Perform an ECG
- Treat any arrhythmia as appropriate
- Admit for observation if loss of consciousness, cardiac arrest, cardiac or respiratory history, arrhythmia or conductive injury
Bactroban
This should be used for routine burn dressings or occlusive bags. Vaseline is adequate for exposure of clean areas such as the face.
Topical application should not be applied to patients being transferred to the burns unit.
Toxic Shock Syndrome ( TSS )
Septicaemia (usually staphylococcal) can occur from surprisingly small burns or scalds in young children. This unusual but potentially lethal complication manifests with high fever, malaise, diarrhoea and vomiting, conjunctival and mucosal injection, a macular rash, and ultimately septic shock. The child should be treated as for septic shock. More on TSS.