This guideline does not apply to immunocompromised or clinically unwell children.
Background
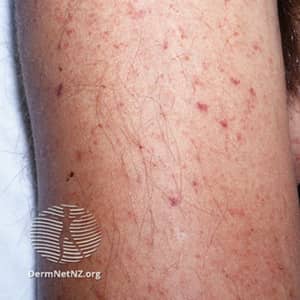
- Petechiae are small (<2mm) purple/red/brown spots which do not blanch under pressure
- Purpura are larger non-blanching spots (>2mm)
- Both can appear in clusters and may look like a fine rash
- They are flat and do not itchy
- >95% of children with fever and petechiae will not have invasive bacteraemia (i.e. meningicoccal or pneumococcal), this refers to immunised children only
This guideline does not apply to immunocompromised or clinically unwell children.
Aetiology
Bleeding into the skin or mucosa from capillaries. This may be from:
Mechanical causes:
- Vagal manoeuvres (coughing, straining, vomiting)
- ↑venous pressure (BP cuff, tight clothing)
- NAI (Slap/hitting can cause localised petechiae)
Infection:
- Bacterial: Neisseria Meningitidis (most common serious bacterial cause), S. pneumoniae, H. influenza, Gp A Strep
- Viral illnesses (enterovirus, influenza)
- Returned traveller – dengue
Risk factors sepsis
- Unwell looking child
- Immunocompromised
- Rapidly progressive symptoms
Clinical
Symptoms
- Non-itchy, non-blanching rash
Signs
- Trauma
- Hepato / splenomegaly
- Lymphadenopathy
- Artheritis
- Abdo. tenderness
Differential Dx
Investigations
- FBC + Film
- CRP
- Clotting
- Blood gas
- Glucose
- Cultures
- Meningococcal PCR
- Consider LP
Management
Discharge criteria
- No progression of rash after 4 hours
- Clinically well
- Bloods normal
- Reviewed by registrar / consultant