Background
Trigger finger presents with discomfort in the palm during movement of the involved digits. Gradually, or in some cases acutely, the flexor tendon causes a painful click as the patient flexes and extends the digit. The patient may present with a digit locked in a particular position, usually in flexion, which may need gentle passive manipulation into full extension. Spontaneous resolution of symptoms can occur in patients with trigger thumb.
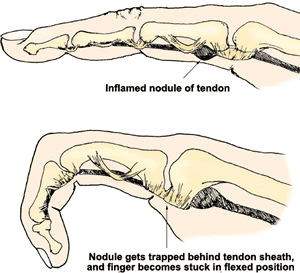
Trigger finger is caused by inflammation and constriction of the retinacular sheath through which the flexor tendons run as they pass from the palm of the hand into the finger. This causes irritation of the tendon, sometimes resulting in the formation of a nodule, which impinges on the pulley, causing pain and restricting movement.
The retinacular sheath is composed of five annular “pulleys” which hold the tendon close to the bone and are integral to the biomechanics of finger flexion. The A1 pulley, at the level of the metacarpal head, is the first part of the sheath and is subject to the highest force.
Epidemiology
- 28 cases per 100 000 population per year = lifetime risk of 2.6%
- This rises to 10% in patients with diabetes
- Diabetic patients are less likely to respond to conservative treatment
- Two peaks in incidence occur:
- < eight yrs (F:M = 1:1). Thumb effected in 90%
- >50 yrs (F:M = 6:1). Finger or thumb effected
- Repetative injuries/occupation
Pathophysiology
- Discrepancy in the diameter of the flexor tendon and its sheath at the level of the metacarpal head
- High pressures occur on maximal flexion and during tight grip
- Recurrent microtrauma causes tendon and sheath hypertrophy
- The narrowed tunnel obstruction usually overcome by powerful flexors
- Weaker extensors unable to counteract
Clinical exam
- >50yo, ♀, Hx DM, dominant hand
- Triggering ↑ by repetitive movements
- If ever locked in flexion (more severe)
- Check all digits as may be multiple
- Palpate for nodule over palmer MC heads
- Check for carpel tunnel (Tinel's / Phalen's signs)
- Corticosteroid injection into the tendon sheath is usually the first line treatment
Management
Options include A) Splint B) Steroid injection C) Surgical release.
Advise light duties. NSAIDs may be of tranisent analgesic use at nodule site.
Splint
- Splint for 6/52 may improve local nodule inflammation.
- Success rates for splintage range from 50% to 70%
- Patients with longer duration of symptoms were less likely to benefit from splintage
Steroid
- Do not use steroid injection in rheumatoid patients (may need tenosynovectomy)
- Single steroid injection is successful in >90% of patients with a palpable nodule or with symptoms present <6/12
- The steroid should be injected around the A1 pulley, not into the tendon.
- Chlorhexidine wipe
- Skin bleb of LA at distal palmer crease
- 25gauge needle, 1ml triamcinolone (10 mg in 1 ml) into the sheath (mobilise finger with needle in situ to ensure not intratendon)
Surgery
- Refer to a plastic hand surgeon (surgical release) if the first steroid injection is unsuccessful or if the finger is locked in flexion
- Percutaneous trigger release (under LA) is safe and effective
Treatment in children
- Children represent a distinct group of patients
- The thumb is involved in 90% of cases
- Good results (50%-80% success) can be obtained with physiotherapy with or without splintage
- Success rates seem to be higher in younger children
Links
How to inject a trigger finger BMJ 2013