Mx of suspected ACS in Munster
Inter-hospital STEMI Transfers
STEMI patients requiring emergent transfer from a non Primary Percutaneous Coronary Intervention (PPCI) Centre (e.g. MUH) to a PPCI Centre (e.g. CUH) are "time critical".
Please quote “CODE STEMI” to ambulance control when requesting such a transfer (details).
Code STEMI should only be used for:
- STEMI patients that have not been thrombolysed, who are being transferred for emergency PPCI or
- STEMI patients thrombolysed that have not reperfused and require emergency rescue PCI
ECG Criteria
- New ST⇑ at J point in 2 contiguous leads of >0.1 mV in all leads other than V2-V3
- For leads V2-V3 the following cut points apply:
- ≥0.2 mV in men ≥40yrs
- ≥0.25 vM in men < 40yrs
- ≥0.15 mV in women
- Other conditions which are treated as STEMI:
- New or presumed new LBBB
- Isolated posterior MI
- The presence of reciprocal ST depression helps confirm the Dx
Posterior MI: ECG changes are: dominant R in V2 with ST depression.
With infarction, the initial ECG may be normal (in up to 30% of cases) [Bestbets]. All patients with an MI history (normal first ECG) need a repeat ECG every 10-15 min, while the patient still has pain, despite analgesia. The patient will either develop changes (i.e. infarct) or the pain will settle with no change in the ECG (unstable angina or a non-Q-wave infarct).
If a pain-free patient develops further pain, repeat the ECG.
General management
Pre-hospital
- Oxygen therapy- continue at 2 Litres/min
- Aspirin 300mg chewed and swallowed, as early as possible [Bestbets]. If this has not occurred, then administer in the ED (the only contraindication is anaphylaxis!)
- Aspirin can be given PR if the patient is vomiting
Emergency department
- Aspirin (as above if not already given)
- PO Brilique 180mg
- GTN spray (400-800 µg) or Suscard Buccal (2mg or 5mg)
- Morphine 2.5-5 mg titrated to the patient's response
- In cases where there is continued or recurrent pain, it is worth considering iv β-blockers (1-10mg Atenolol titrated to pain)
- Β-blockers are contraindicated in:
- heart failure, asthma or bronchospasm, heart block, HR<50, SBP< 90mmHg
Thrombolysis contraindications
Absolute contraindications
- Active internal bleeding
- CVA within 6 months
- Cranial or spinal surgery within 2 months
- Cerebral or spinal tumour or AV malformation
- BP >200/120 not amenable to ED treatment
- Severe bleeding problem
(moderate, such as Von Willebrand's acceptable)
* Angioplasty is an alternative when there is a contraindication to thrombolysis (discuss with duty cardiologist).
Relative contraindications
- Cerebro-vascular disease
- Gastrointestinal or urological bleeding within 10/7, including puncture of non compressible vessels
- BP >180/110
- Suspected left heart thrombus (i.e. mitral stenosis with AF)
- Suspected aortic dissection or pericarditis
- Infective endocarditis
- Known coagulation defect (inc. severe liver disease)
- Pregnancy
- Active haemorrhagic ophthalmic disease
- Warfarin (manufacturers' recommendation; no data)
- For rPA, age >75, small infarctions, MI onset > 6hrs
Informed consent
The main risk of thrombolysis is haemorrhage and the patient must be made aware of this prior to treatment.
The risk of CVA is 4/1000 treated above normal incidence for SK, 9/1000 for rPA. (Note: half of each of these die - it's a haemorrhagic stroke). The risk of non-cerebral bleed is 7/1000 patients treated.
Troubleshooting
Treatment of hypertension
- Ensure adequate analgesia
- In the first instance, try 800 mcg (2 puffs) GTN
- iv B blockade (see above)
- iv Nitrate infusion(or Buccal Suscard)
Complications of thrombolysis
Hypotension
If SBP<90mmHg then:
- Tip the patient "head down"
- Administer 250ml saline
- Slow the infusion down, or stop temporarily
- If marked bradycardia then Atropine 0.6-1.2mg iv
Reperfusion arrhythmias
Common, generally short (and therefore non-sustained) runs of VT or idioventricular rhythm.
- Consider Lidocaine if problematic
- Cardiac arrest - follow the ALS protocol
- Heart block - acute myocardial infarction can be associated with any degree of heart block. If haemodynamically stable and asymptomatic, observe closely but continue treatment and seek senior advice so that pacing can be considered
- Treat the bradycardia according to the ALS peri-arrest protocols
Allergic reactions
- Stop the infusion
- Hydrocortisone 200 mg and
- Chlorpheniramine 10 mg as iv injections
Bleeding
Minor haemorrhage - compression.
For larger bleeds -
- Stop thrombolysis
- Resuscitate
- Call for ED senior help
For catastrophic bleeds (massive GI or intracranial)
- Stop thrombolysis
- FFP (4 units) and packed cells
- Consider Tranexamic Acid (TXA) 10mg/kg
- Consider Protamine 10mg/1000iu heparin infused / SC to a max of 7.5 ml (75mg)
If the patient develops neurological symptoms then an immediate CT scan is required
In CUH: Tranexamic Acid injection - TXA- (Cyklokapron) is kept in the Haematology section of the drugs cupboard in Resus., and in the clean utility room behind the Nurses Station. TXA infusion guide.
Thrombolytics
Alteplase (tPA)
15mg IV bolus
0.75 mg/kg IV over 30 min (up to 50mg)
Then 0.5 mg/kg IV over 60 min (up to 35mg)
Tenecteplase
Single IV bolus:
- 30mg (6000 IU) if <60kg
- 35mg (7000 IU) if 60-70kg
- 40mg (8000 IU) if 70-80kg
- 45mg (9000 IU) if 80-90kg
- 50mg (10000 IU) if ≥90kg
- Reduce to half-dose in patients ≥75 years of age
Unfractionated heparin
UFH (not LMWH) 60 IU/kg IV bolus with a maximum of 4000 IU followed by an IV infusion of 12 IU/kg with a maximum of 1000 IU/hour for 24-48 hours. Target aPTT: 50-75 s or 1.5 to 2 times that of control (ESC 2017 guideline, local targets may vary) to be monitored at 3, 6, 12 and 24 hours.
Warfarin
- For patients on warfarin take blood samples for INR and group and save
- This is only a relative contraindication to thrombolysis
- If in doubt discuss with a senior
LBBB and paced rhythms (Sgarbossa criteria)
The diagnosis of MI is complicated in these cases. There are certain features which have been noted to increase the likelihood of a concurrent MI.
ST >1mm elevation in leads where QRS is positive (V5 V6)
ST >5mm elevation in leads where QRS is predominately negative (V1 - V3)
ST depression >1mm V1-V3.
If there are any of the above features treat as a new "thrombolysable" event.
Ask for ED senior help now.
More on LBBB and Sgarbossa criteria.
Continuing care
Thrombolysed patients or those post cardiac catheterisation should receive their ongoing care on the CCU. Transfer to CCU will be arranged by the nursing staff, but the On Call cardiology team must also be informed of the admission.
An inpatient drug chart should also be completed and the following prescribed:
- Opiate analgesia
- Anti emetic
- Nitrates
- Aspirin 150 mg od
- Heparin for DVT prophylaxis (either unfractionated Heparin 5000 iu bd or Enoxaparin 20mg od) in patients given Streptokinase
ECG examples
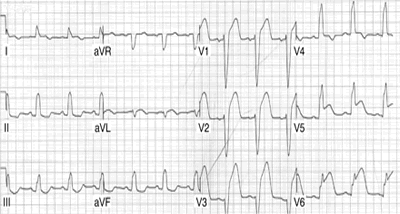
Anterior AMI
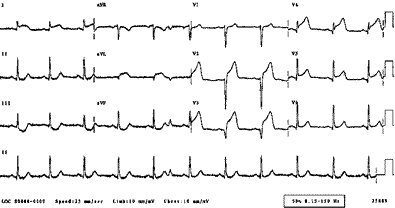
Inferior AMI
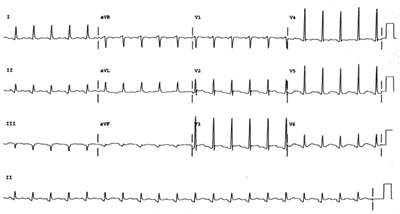
Posterior AMI
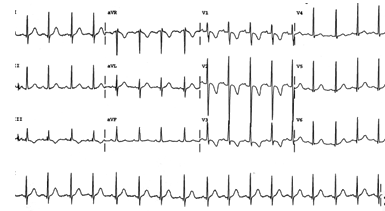
Sgarbossa Criteria (See below)

LBBB and paced rhythms (Scarbossa criteria)
The diagnosis of MI is complicated in these cases. There are certain features which have been noted to increase the likelihood of a concurrent MI:
- ST >1mm elevation in leads where QRS is positive (V5 V6)
- ST >5mm elevation in leads where QRS is predominately negative (V1 - V3)
- ST depression >1mm V1-V3
If there are any of the above features treat as a new cathglab/thrombolysable event.
Ask for EM senior help now.